A single stalled claim costs you more than just the delay. Every day between FNOL and Settlement erodes policyholder trust, inflates Loss Adjustment Expenses, and pushes your Net Promoter Score into churn territory. The claims experience is the single biggest driver of retention, yet most insurers are operating blind.
This is not a training problem. This is not a staffing problem. This is a visibility problem.
The hidden cost of workflow blind spots
When you lack continuous, real-time process intelligence, you cannot distinguish between:
- A claim that is moving through the system normally
- A claim that is stuck in a silent bottleneck waiting for a manual exception review
- A claim that has been routed incorrectly and is about to breach your time to settlement targets
Traditional claims management dashboards show you status. They do not show you flow.
The breakdown happens in the transitions
Research shows that the majority of claims processing delays occur not during active work, but in the handoffs between stages:
- Intake to assignment: Claims sit in queues waiting for automatic routing rules that fail on edge cases
- Assignment to investigation: Adjusters receive incomplete documentation and must loop back to request additional information
- Investigation to approval: Manual review workflows create undocumented wait states that are invisible to management
- Approval to payment: Finance systems require manual reconciliation steps that are not tracked in your claims platform
Each of these transition points adds 1-4 days of silent delay. Multiply that across thousands of claims, and you have a systemic 30% efficiency gap that does not appear in any single KPI.
What real-time process intelligence reveals
Namuda does not replace your claims management system. It sits on top of your existing infrastructure and analyzes the digital traces left behind by every claim interaction: case updates, status changes, system handoffs, manual interventions, and exception routing.
By reconstructing the actual process flow, Namuda exposes:
- The real bottleneck locations: Not where you think claims are delayed, but where the data proves they are stalling
- The hidden rework loops: Claims that bounce back between stages due to incomplete initial processing
- The exception handling burden: How many claims require manual intervention, and why automated routing is failing
- The true cost per claim: Operational expenses broken down by process phase, including the cost of delays
Start measuring
Most process improvement initiatives fail because they are based on intuition rather than evidence. Managers assume that the intake phase is slow, so they add headcount. But the data shows that intake is fast; the real delay is in the handoff between intake and assignment, where claims sit in a queue for 2 days waiting for manual review.
Namuda eliminates the guesswork. Every process deviation is tracked. Every bottleneck is quantified. Every improvement initiative is measured against live baseline data.
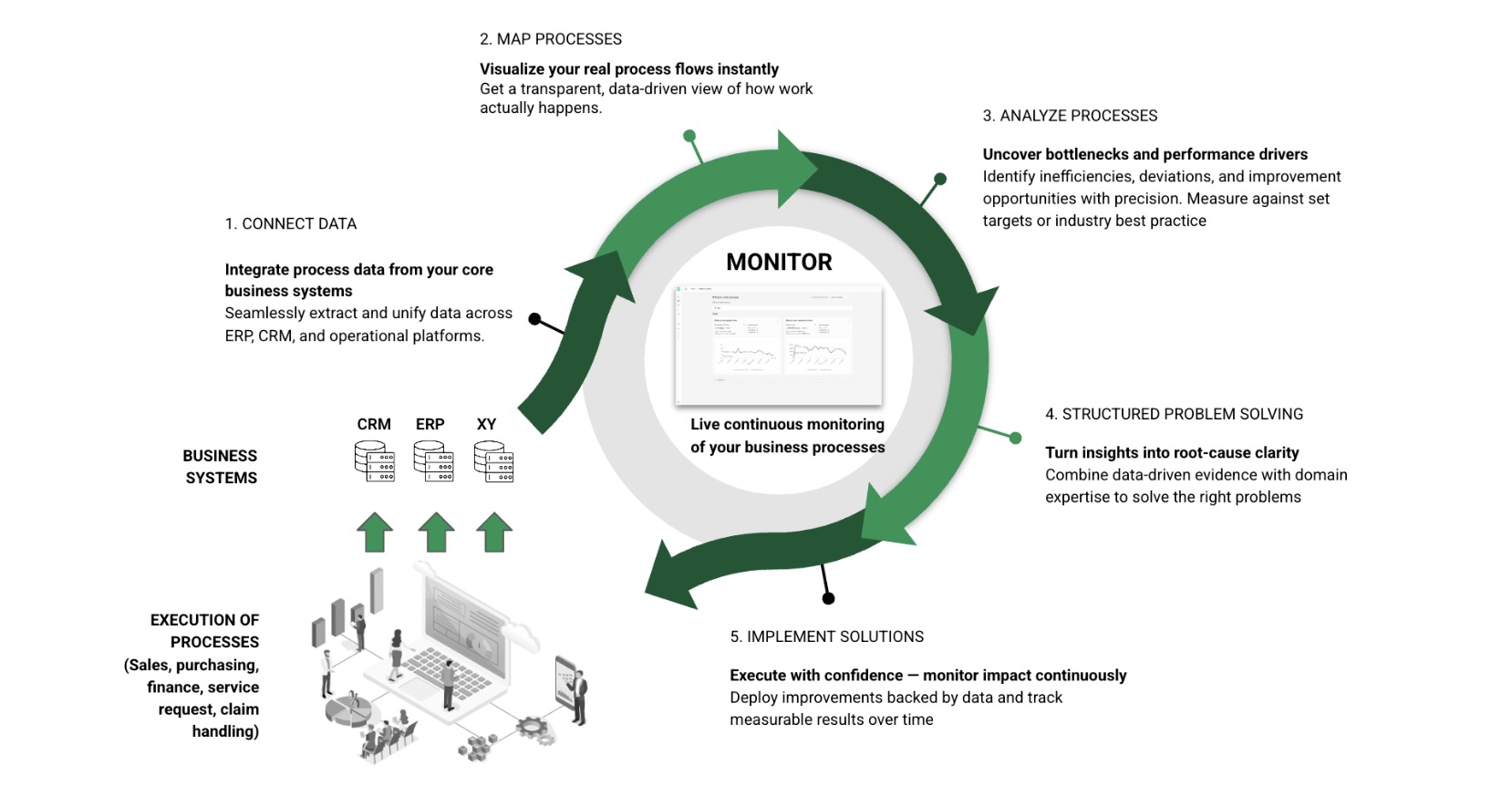
How it works
- Connect your systems: Namuda engineers conect with your existing claims platforms, policy administration systems, and third-party data sources.
- Map the real process: Our system reconstructs the actual flow of every claim, not the idealized process documented in your SOP manual
- Identify the delays: Agentic analysis pinpoints exactly where claims stall, why they deviate, and starts root cause analysis.
- Track improvements: As you implement changes, Namuda continuously measures the impact on cycle time, rework rates, and cost per claim
The claims experience is your retention lever
A bad claims experience is the number one driver of policyholder churn. When a claim takes too long, when communication is inconsistent, when policyholders have to call multiple times to check status, they leave.
Namuda ensures that every policyholder interaction is backed by optimized workflows. By eliminating silent delays and hidden bottlenecks, you accelerate payouts, reduce frustration, and turn claims processing into a retention advantage rather than a churn risk.
Ready to accelerate your claims cycle?
The difference between a 28-day claims cycle and a 19-day claims cycle is not more staff or better software. It is continuous visibility into where the process actually breaks down, and the ability to fix it permanently.
Start off with a 2-week process scan to reveal the most severe root causes of inefficiency.
Every exception and manual workaround adds cost.
Namuda detect non-standard paths before they become systemic.

.png)